Sepsis
What is sepsis?
Bacteria in the blood (bacteraemia) can cause sepsis, previously known as blood poisoning. This is a syndrome involving life-threatening organ failure caused by a dysfunctional systemic immune response. Anyone can develop sepsis as a consequence of a common bacterial infection, such as a urinary tract infection or pneumonia. The need for rapid and reliable diagnostics to enable proper treatment for severe conditions such as sepsis is crucial for patient survival. The initial main application for the ASTar system will be the analysis of positive blood cultures from patients with suspected sepsis.
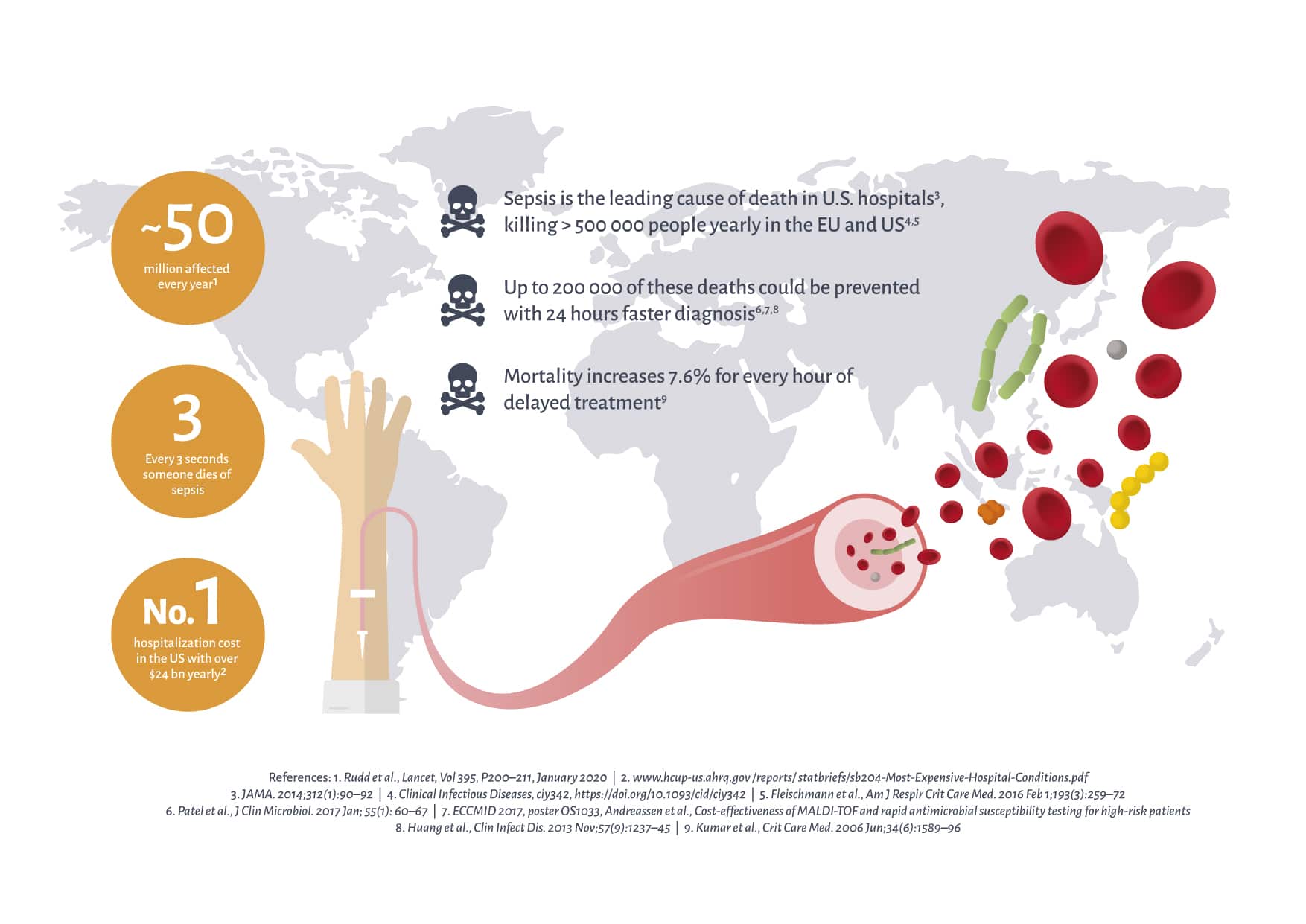
Sepsis is a global health problem, afflicting up to 50 million people every year. In several studies, mortality from sepsis has been measured between 15 and 50%, with the higher end of that range relating to patients in septic shock. In the case of sepsis, every hour that effective treatment is delayed may have a devastating effect. Mortality for patients who develop septic shock increases by 7.6% for each hour without correct antibiotic treatment (Kumar et al. Crit Care Med. 2006).
In the US, it is reported that approximately two million people suffer from sepsis every year, about 250,000 of whom die from the disease. The incidence and mortality of sepsis are similar in the EU. Overall, this means that the number of sepsis deaths exceeds the total number of deaths due to breast cancer, prostate cancer and colon cancer in the same countries.

Antimicrobial resistance – a growing threat to human health
Healthcare is currently dependent on the use of effective antimicrobials, for example in surgical procedures, transplants and cancer treatments, which entail a greater risk of infection. If the development of antimicrobial resistance is not stopped, it will pose a serious threat to healthcare and one of the biggest threats to human health.
It is shown that the more antimicrobials used, the faster the increase in antimicrobial resistance. It is also recognised that resistance has developed against every new antimicrobial that has been introduced. Furthermore, there are few new antibiotics under clinical development. According to a recent report by WHO, most antimicrobials under development are modifications of older types of antimicrobials, which is why resistance to these antimicrobials develops rapidly.
The most beneficial and cost-effective treatment strategy, for both the individual patient and for society, is to invest in new, faster diagnostics. Rapid diagnostics shorten the time to optimal patient treatment, resulting in reduced use of broad-spectrum antimicrobials. This involves several advantages, including curbing the trend of resistant bacteria, reducing patient suffering, as well as reducing the number of treatment days which significantly cuts costs for hospitals, the healthcare sector and society in general.
There will be a need for new classes of antimicrobials and it is crucial that diagnostics systems can be easily adapted to include also these in their antimicrobial panel, a feature that ASTar provides.

Help sepsis patients quickly return to everyday life

